The Weight You Can’t See: Looking Beyond Sadness in Depression
Depression Is More Than Feeling Sad
Some difficulties cannot be seen on surface level. A person can seem completely fine (going to work, taking care of himself replying to messages), while internally feeling anchored down by something can’t fully explain. Depression is often mistaken as just sadness or personal weakness, yet it is a complex clinical condition that alters how a person thinks, feels, behaves, and even functions physically. It commonly is seen as persistent low mood, loss of interest in previously enjoyable activities, reduced energy, disrupted sleep or appetite, difficulty focusing, and recurring feelings of guilt or hopelessness.

The Brain–Behaviour Connection
Changes in the communication between various brain regions are associated with depression.
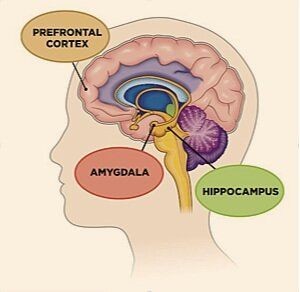
The “prefrontal cortex handles rational thinking and regulating emotions”, may struggle to effectively manage persistent negative thoughts. At the same time, the “amygdala, which is the brain’s emotional alarm system”, can become overactive, amplifying distressing experiences.
The “hippocampus, another important part, helps in memory and control of stress reactions” Prolonged stress can interfere with its functioning, possibly weakening its ability to regulate memory and stress responses. In addition, the “Default Mode Network, a system active during self-reflection” which may become over engaged, “contributing to cycles of rumination and repetitive negative thought patterns”.
When combined, these alterations may cause the mind to become less receptive to positive experiences and more sensitive to negative ones.
Another thing that is physiologically altered in “encoding of memory”. It means that what we see at present is understood and stored as short term memory which is affected. In depression the affected areas prefrontal cortex, amygdala and hippocampus, this is something people with depression undergo and are not able to stay in present leading them to constantly think of the negative situations that they have encountered throughout their lives.
When Motivation Fades
Decreased motivation and enjoyment is one of the pointers of depression. This is intricately linked to disruptions in the “brain’s reward system – dopamine” which is a neurotransmitter.
When dopamine signalling is altered, everyday responsibilities may feel exhausting, and activities that once brought pleasure may no longer feel rewarding. As a result, advising someone to “just stay positive” or “try harder” overlooks the underlying biological changes shaping their experience.
What Leads to Depression?
Depression rarely develops from a single cause. It usually emerges from a combination of stressors and individual susceptibility.
Common stressors include:
- Ongoing stress
- Bereavement or loss
- Trauma
- Interpersonal conflicts
- Medical conditions
- Major life transitions
However, exposure to stress alone does not guarantee depression. Individual vulnerability plays a crucial role.
Understanding Vulnerability
“The diathesis–stress framework offers one explanation for why similar stressors affect individuals differently”, leading some to develop depression while others stay resilient. According to this model, depression appears when pre-existing or premorbid vulnerability interacts with significant life stress.
Vulnerability could result from:
- Genetic elements, like hereditary
- Stress-response systems’ biological sensitivity
- Psychological characteristics, such as perfectionism or self-criticism
- Early life events, like hardship during childhood (sexual, emotional or physical)
The body’s stress pathway is triggered by prolonged stress, which raises cortisol levels. Over time, this may have an impact on mood and memory-related brain areas, worsening depressive symptoms.
Recovery Is Possible
Importantly, the brain owns a capacity for adaptation known as neuroplasticity—the ability to reorganize and form new connections over time. Therapeutic interventions can enhance emotional regulation and promote healthier thought patterns. Neurotransmitter balance may be supported by medications. Recovery is also influenced by lifestyle elements like regular sleep, exercise, and social interaction.
Depression is not a reflection of personal weakness; rather, it arises from a complex interplay between biological systems, individual vulnerability, and lived experience. Healing is possible with the correct support, even though the burden may not be clear to others.
